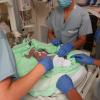
BC Children’s hospital and BC Women’s Hospital & Health Center have many available experts and resources to address reproductive infectious diseases (RID), affecting mothers and their infants. However, up until now these services were siloed in their respective hospitals. Mothers with RID delivered at BC Women’s and their infants born with congenital infections received their care at BC Children’s. Lead by Dr Chelse Elwood and with the help of the Joint Collaborative Committees (JCC)’s Health System Redesign (HSR) project, both the RID and Pediatric Infectious Disease programs are transitioning into one space – the Oak Tree Clinic (OTC).
Passion project saves lives of those in respiratory crisis
When Dr Hussein Kanji decided to develop expertise in the Extra Corporeal Membrane Oxygenation machine -- or ECMO -- as his “passion project”, he had no way of knowing that it could be a lifeline d
Spotlight on a Specialist: Dr Andrew Krahn
Dr Andrew Krahn, Head of UBC Cardiology and a cardiologist at St Paul’s and Vancouver General hospitals, is a leader in genetically related heart disease. His journey to his current position started by following his own heart. Originally, leaning towards studying engineering, he veered at the last minute to taking undergraduate sciences that eventually led to a career in medicine.
BC doctors join the Institute for Healthcare Improvement’s annual forum virtually
Over the last five years, the Specialist Services Committee (SSC) and Shared Care Committee (SCC) has funded BC doctors to attend the Institute of Healthcare Improvement’s (IHI) annual forum in Orlando, the world’s premier healthcare event that attracts thousands of health care participants from across the globe, providing them with inspiration, networking, and knowledge sharing opportunities. Adapting to the travel and gathering restrictions caused by the COVID-19 pandemic, the event was hosted virtually last December (6-9) with 128 participants from BC sponsored by SSC and SCC.
Introducing the new SSC Co-Chair, Dr Ahmer Karimuddin
Representing Doctors of BC on the Specialist Services Committee (SSC) as the new Co-Chair, Dr Ahmer Karimuddin, a general and colorectal surgeon, is a familiar face on SSC, the Joint Collaborative Committees (JCCs), and Doctors of BC.
Registration open for online course on Finding and Creating Joy in Work
Given the popularity of the course on Finding and Creating Joy in Work among the participa
Physician project cuts patient wait times by half
Patients who are getting bloodwork done at the outpatient lab in the Gordon and Leslie Diamond Health Care Centre are no longer facing lengthy wait times, with the introduction of new online booking system that allows appointments to be made ahead of time. The project is another example of advancements supported by the Physician Quality Improvement (PQI) initiative, to improve the quality of health care for British Columbians.
Helping to change the paradigm of treatment for alcohol use disorder in BC
When Dr Jeff Harries first read in a 2003 Lancet article about a pharmacotherapy that helped some patients with alcohol use disorder (AUD), it began a change in how he understood AUD.
Funding support available for BC doctors to attend Quality Forum
BC doctors are invited to join the annual Quality Forum on February 25 and 26, 2021.
Leveling the playing field for osteoporosis care
A Canadian study conducted in 2014 found that more than 320,000 hip fractures occur in North America each year and the death rate within a year of surgery ranges from 14 to 36 per cent -- fractures
Specialist Services Committee Backs Expansive Strategy For Improving Cystic Fibrosis Patient Care
This article was first published in the BC Medical Journal's November 2020 edition.
COVID-19 Office Safety Plan Support Grant for BC’s Community Physicians
Doctors with community offices in BC have invested time and expense to re-open their practices in a way that ensures safe in-person care for patients.
To help offset some of these costs, the Joint Collaborative Committees – a partnership of Doctors of BC and the BC government - are reallocating funds to provide a $1,000 grant to each eligible physician who has implemented COVID-19 Safety Plan in their community practices.
Spotlight on a Specialist – Dr Tiffany Chan
Campbell River’s colorectal surgeon, Dr Tiffany Chan, chose her path by following this piece of advice: pick a speciality with the kind of people you like to hang out with because they will be your colleagues, mentors and advisors for the rest of your career. Dr Chan found that colleagues in colorectal surgery were her kind of people.
Doctors unite to fight incorrect diagnoses of penicillin allergy
Approximately 10 per cent of patients in BC’s medical system believe they’re allergic to penicillin, but 90 per cent of those patients are wrong.
“It’s a big problem because people are getting antibiotics that aren’t optimal for their therapy, and it’s costing the health care system quite a bit of money,” says Dr Tiffany Wong, an allergist in the Division of Allergy and Immunology at BC Children’s Hospital.
BC specialists and family doctors sponsored to participate virtually at the IHI National Forum
The Specialist Services and the Shared Care Committees are pleased to sponsor 100 specialists and 100 family physicians in BC
Island Health blazes a new trial by cutting back on MS patients’ need to travel for care
The success of Island Health’s RuralHealth TeleMS program can be measured in kilometers not driven, time not spent commuting, gas dollars saved, and energy retained by patients whose Multiple Sclerosis (MS) already depletes their resources.
Community Specialists: We are looking for your input
Various community-based specialists have approached us at the Specialist Services Committee (SSC) about the hurdles that you encounter as you work to provide the best possible patient care. To ensure we have a broad understanding of these challenges, we need your input. Please fill out this five-minute survey by September 25,2020. The survey outcomes will be used to inform our ongoing work and will help us address your needs, so that together we can help improve patient care in BC.
Teamwork is delivering powerful changes for newborns
Dr Sandesh Shivananda, Medical Director at the BC Women's Hospital Neonatal program has seen many significant changes in quality of care and teamwork since moving in the new Teck Acute Care Centre in 2017 – a centre with 70 beds that provides birth and post-birth care for mothers and new born babies.
Registration open for online course on Finding & Creating Joy in Work
Given the popularity of the course on Finding and Creating Joy in Work among the participants over the last year, the Specialist Services and Shared Care Committees via their Physician Leadership S
Spotlight on a Specialist - Dr Carol Ward
Dr Carol Ward, a geriatric psychiatrist chose her specialty for the opportunity to connect with people. “I love stories. I love to hear people’s stories. And the longer you live, the better the story.” Growing up in the Maritimes, Dr Ward was surrounded by good story-tellers – “Generally speaking I find older folk are grateful and very appreciative of being able to share their lived experience.” Knowing her patients’ stories is her way to helping them. Dr Ward finds that it’s like being a detective – pulling all aspects of medicine and a person’s background together.